More fear than harm
- Paediatric dermatology
-
The clinical case
-
Now it's your turn!
-
Co-prescription and advice
Clinical case presentation
A 13-month-old infant with no previous history of illness presented to the emergency room with febrile purpura 15 days after a hand-foot-and-mouth disease (Coxsackie infection) and 10 days after a third injection of hexavalent vaccine.
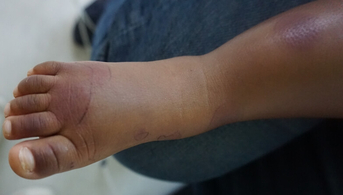
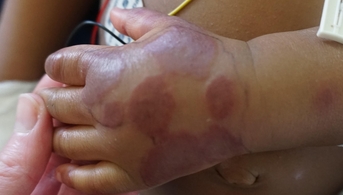
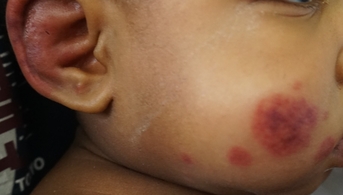
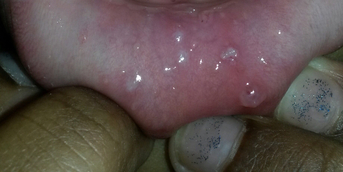
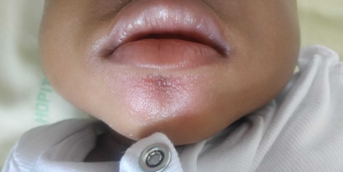
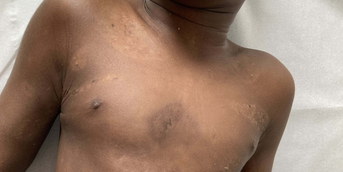
The rash appeared in the late afternoon in a healthy child, but the appearance of a fever during the night worried the parents. It consisted of large, infiltrated, purpuric nummular lesions on the hands and feet, ecchymotic on the cheeks and ears, associated with painful edema of the same areas. The child was transiently subfebrile at 37.8°C, but his neurological and hemodynamic status remained perfectly reassuring.
Biological tests showed normal liver and kidney function, and a very moderate inflammatory syndrome (CRP 20) with no hematological abnormalities. Ceftriaxone 100 mg/kg was given immediately, and the child was transferred to intensive care for monitoring.
Your turn
What is your diagnosis?
Select 1 answer(s) from the following choices:
Wrong answer!
Good answer!
Selected diagnosis
This is a typical case of acute hemorrhagic edema (AHE) of infancy, a mainly cutaneous vasculitis of very young children whose characteristic lesions allow a purely clinical diagnosis: purpura is always round (annular, targetoid, arcuate or polycyclic), may be papular or ecchymotic, and is localized to the extremities, which are frankly edematous: hands, feet, face and ears, more rarely the genitals. Lesions are fixed, non-pruritic and sometimes painful.
Although some equate AHE with Henoch-Schönlein purpura, extracutaneous involvement is exceptional and the spontaneous evolution is always favorable.
Explanation of wrong answers
- Purpura fulminans is a pediatric emergency that should be suspected and treated as such whenever there is the slightest suspicion of febrile purpura in children, as was the case with this child. This purpura, which occurs during bacterial sepsis (especially meningococcal sepsis), is rapidly progressive and necrotic, and any purpuric element larger than 3 mm in the context of fever and/or shock (tachycardia, hypotension, increased capillary refill time) should be considered suspicious for purpura fulminans.
- Acute urticaria in infants, most often caused by viruses, is often annular, polycyclic and ecchymotic in terms of course. It lacks the acral distribution and marked edema of AHE, but is its main differential diagnosis.
- Acquired protein S deficiency occurs in young children following a viral infection (usually varicella) due to the production of cross-reactive antibodies between the varicella-zoster virus (VZV) and protein S. It is an even rarer pediatric emergency than purpura fulminans, with ecchymotic lesions, sometimes necrotic purpura, multiple thromboses and laboratory features of disseminated intravascular coagulation.
Treatment
None.
The evolution was spontaneously favorable: 24 hours later, the child's clinical condition was stable and the test for proteinuria was negative. A return home was therefore authorized.
Message from the expert
Acute hemorrhagic edema of infancy is a concerning dermatosis due to its purpuric nature. It is clinically easy to diagnose in its typical form, but is probably over-diagnosed in cases of acute ecchymotic urticaria, which is much more common in this age group.
References
Bronz G, Rinoldi PO, Lavagno C, Bianchetti MG, Lava SAG, Vanoni F, Milani GP, Terrani I, Ferrarini A Skin Eruptions in Acute Hemorrhagic Edema of Young Children: Systematic Review of the Literature.Dermatology. 2022;238(3):397-403
Find your clinical cases
Want to read on?
This access is reserved for professionals, registered on Pierre Fabre For Med.
To access the full content, please register or log in if you already have an account.