Lumps behind the ears
- Dermatology on pigmented skin
-
The clinical case
-
Now it's your turn!
-
Co-prescription and advice
Clinical case presentation
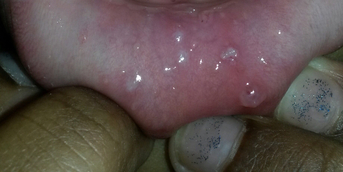
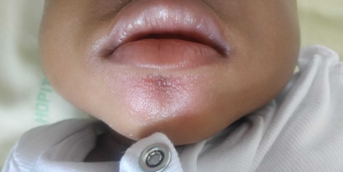
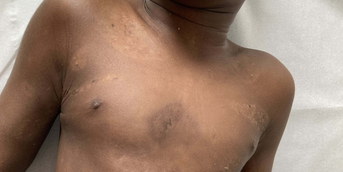
Three months after the onset of a large right retroauricular lymphadenopathy, this 14-year-old adolescent, who regularly stayed in Senegal, presented with a left retroauricular dermatosis: subcutaneous papulonodules grouped into a noninflammatory, fixed, slowly progressive plaque.
The lymphadenopathy had not only persisted but also increased in size (3 cm in diameter). It was mobile, painless and solitary, and the remainder of the physical examination was unremarkable.
An initial screening workup, as well as extensive hematologic and infectious investigations, were normal except for eosinophilia at 800 cells/mm³ and elevated IgE at 1120 in this nonatopic patient.
The skin biopsy showed a dermal inflammatory infiltrate composed predominantly of lymphocytes, but also containing a few eosinophilic polymorphonuclear cells. It was the histologic analysis of the lymph node, which was completely excised, that allowed a diagnosis to be made.
Your turn
What is your diagnosis?
Select 1 answer(s) from the following choices:
Wrong answer!
Good answer!
Selected diagnosis
Associated with follicular hyperplasia, there was a significant diffuse infiltration of the lymphoid tissue by eosinophilic polymorphonuclear cells and vascular hyperplasia with vessels surrounded by hyaline fibrosis. This angiolymphoid hyperplasia with eosinophilia is suggestive of Kimura disease. This diagnosis was therefore retained on the basis of several additional arguments:
- Patient profile: young man
- Retroauricular topography of the lymph node involvement (enlarged adenopathy) and skin involvement (subcutaneous nodules)
- Th2 biological signature (hypereosinophilia, elevated IgE)
The staging workup was limited to screening for proteinuria, as Kimura disease can be complicated by nephrotic syndrome.
Explanation of incorrect answers
- Cutaneous and nodal sarcoidosis was clinically compatible but did not explain the laboratory abnormalities. It was ruled out by histology (no granulomas).
- The same arguments ruled out cutaneous tuberculosis.
- Cutaneous leishmaniasis is often crusted or ulcerated and is not accompanied by reactive lymphadenopathy unless there is secondary infection.
Treatment
A watchful waiting/monitoring approach was decided in a multidisciplinary team meeting because of the indolent nature of the skin lesions and the absence of visceral involvement.
Surgery may be proposed in cases of troublesome skin lesions, but postoperative recurrences are not uncommon.
In disabling forms or in cases progressing toward systemic involvement, systemic corticosteroid therapy remains the first-line treatment.
Expert's message
A large chronic lymphadenopathy without a documented infectious cause must be biopsied to rule out a hematologic malignancy (lymphoma) or a proliferative disease (sarcoidosis, Kimura disease, etc.).
References:
Yumiao Mai et al. Kimura disease in children: A report of 11 cases and review of the literature. Front Pediatr. 2023;11:1131963
Find your clinical cases
Want to read on?
This access is reserved for professionals, registered on Pierre Fabre For Med.
To access the full content, please register or log in if you already have an account.