Rapidly progressive cutaneous infiltration
- Adnexal diseases
-
The clinical case
-
Now it's your turn!
-
Co-prescription and advice
Clinical case presentation
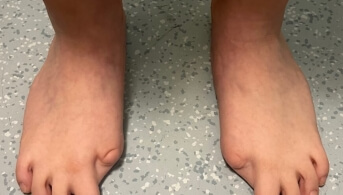
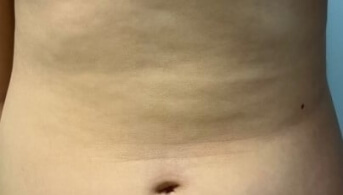
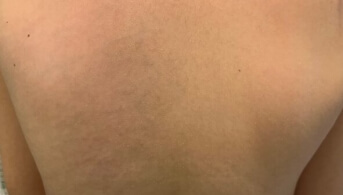
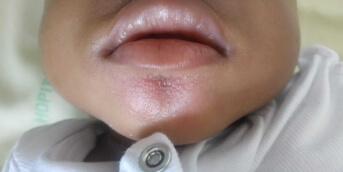
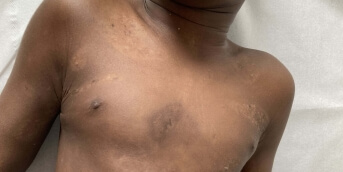
An 11-year-old pre-adolescent girl presented to the emergency department with rapidly progressive sclerotic edema of the trunk, causing significant pain and functional impairment. Her only past medical history was congenital agenesis of both great toes, which had never been investigated in her country of origin.
Within a few days, indurated plaques of the trunk and limb roots developed spontaneously. They were very hard, painful to the touch and warm. This “corrugated iron” rather than “peau d’orange” appearance caused stiffness, scoliosis, limitation of cervical mobility in all planes as well as inability to raise the left upper limb. She had no systemic or extracutaneous signs, no biological inflammatory syndrome, no blood hypereosinophilia, and a comprehensive infectious workup was negative.
Ultrasound and MRI confirm heterogeneous hypodermal and muscular infiltration of the areas involved. X-rays of the extremities showed exostoses, demineralization and abnormalities of the metatarsals and phalanges, which helped guide the diagnosis and avoid a skin biopsy.
Your turn
What is your diagnosis?
Select 1 answer(s) from the following choices:
Wrong answer!
Good answer!
Final diagnosis
The clinical and radiological congenital abnormalities of the great toes in this patient made it possible to attribute this inflammatory sclerotic edema to a first flare of fibrodysplasia ossificans progressiva.
This autosomal dominant genetic disease (mutation of the ACVR1/ALK2 gene) combines a pathognomonic congenital malformation of the great toes with episodes of soft tissue edema that will progressively evolve toward ossification of striated muscles, fascia and tendons, hence its name “stone man disease.”
Flares are triggered by any physical trauma (blows, injuries, falls, invasive iatrogenic procedures) as well as viral infections. Skin biopsy should therefore be avoided whenever possible. Symptomatic treatments, mainly anti-inflammatory, are minimally or not effective and trials of innovative therapies are underway to prevent progression toward generalized ankylosis with respiratory failure.
Explanation of the incorrect answers
- Bacterial dermohypodermitis was rapidly ruled out by the absence of erythema, fever, elevated inflammatory markers and any portal of entry for infection.
- Shulman fasciitis is considered a subtype of deep morphea, characterized by frequent blood and/or cutaneous hypereosinophilia and a dimpled “groove sign” or “valley sign” appearance that is highly suggestive. It is very rare in children and is not associated with congenital bone abnormalities.
- Buschke scleredema presents as diffuse symmetrical induration corresponding to deep dermal mucin deposits (histological diagnosis). It does not involve muscle. It has been described in association with diabetes in obese men, and in young women, adolescents and children following streptococcal upper respiratory tract infections.
Treatment
Trials of innovative therapies at a specialized reference center.
Expert’s message
The presence of congenital great toe abnormalities should suggest fibrodysplasia ossificans progressiva in any case of painful cutaneous infiltration, in which case skin biopsy would be contraindicated.
References:
Understanding the clinical morbidity and mortality of fibrodysplasia ossificans progressiva: a systematic literature review.
Harrak H, Rhee S, Souttou A, O'Meara SJ, Knox C. Orphanet J Rare Dis. 2025 May 31;20(1):262.
Find your clinical cases
Want to read on?
This access is reserved for professionals, registered on Pierre Fabre For Med.
To access the full content, please register or log in if you already have an account.