A far-fetched story
- Scalp pathology
-
The clinical case
-
Now it's your turn!
-
Co-prescription and advice
Clinical case presentation
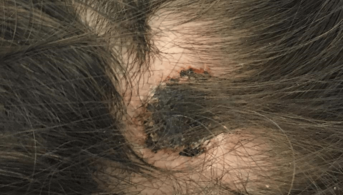
This 8-year-old girl regularly has her hair braided. On the night following the braiding session, she reported to her parents localized scalp pain that increased, prompting the braids to be removed; the scalp, which was initially normal, became erythematous then bullous and pustular within 48 hours, prompting a visit to the emergency room.
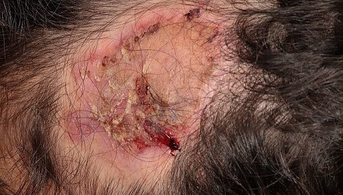
The patient was then treated with amoxicillin and clavulanic acid and a silver sulfadiazine ointment: the inflammatory lesions regressed, giving way to a vast area of scarring alopecia. There was no inflammation or peripilar hyperkeratosis, no specific dermoscopic appearance and the rest of the dermatological examination was strictly normal.
A biopsy was then taken: the histological appearance was that of cicatricial alopecia (absence of hair follicles) with an outline of epidermal detachment and extravasated red blood cells; a mononuclear inflammatory infiltrate with peri-annexal enhancement was also noted. PAS (Periodic Acid-Schiff) staining was negative.
Your turn
What is your diagnosis?
Select 1 answer(s) from the following choices:
Wrong answer!
Good answer!
Selected diagnosis
On further questioning, we learn that just after braiding, the young patient put her helmet on her head to go cycling, which seems to have triggered the first localized scalp pains. The pressure of the helmet on the braids probably accentuated the mechanical aggression on the hair follicle, leading to acute traction alopecia via oedema then ischemia followed by necrosis. A 2021 publication identical in every respect to our own reached the same conclusion.
Traction folliculitis is classic in patients whose hair is often braided very tightly. In the long term it can lead to definitive progressive scarring alopecia; very violent acute traction (accidental or during styling) can lead to follicle necrosis, resulting in acute alopecia.
Explanation of wrong answers
- Ringworm should always be suspected in the presence of any scalp pathology in children. Ringworm causes highly inflammatory necrotic lesions that can rapidly develop into scarring alopecia in the absence of appropriate treatment. In this case the diagnosis is ruled out by negative PAS staining.
- The successive occurrence of painful erythema, then phlyctenae, then crusts and finally scarring alopecia suggests a thermal or caustic burn, but the interview did not reveal any treatment associated with braiding.
- The presence of bullae rather than follicular papules and, above all, the rapidity of evolution are not in favor of lichen planopilaris, which is exceptional in this age group.
Treatment
No treatment is proposed at this stage of scarring alopecia.
Message from the expert
Hair-braiding-induced traction folliculitis is edematous and reversible in most cases but can progress to definitive hair follicle necrosis if the mechanical aggression is too violent or too chronic.
References
Johns HR, Wright TS, Pourciau CY. Acute onset traction-associated ulceration and alopecia. Pediatr Dermatol. 2021;38(Suppl. 2):103-105
Find your clinical cases
Want to read on?
This access is reserved for professionals, registered on Pierre Fabre For Med.
To access the full content, please register or log in if you already have an account.