Acquired keratosis pilaris
- Facial dermatosis
-
The clinical case
-
Now it's your turn!
-
Co-prescription and advice
Clinical case presentation
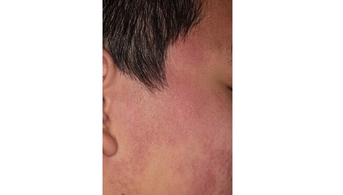
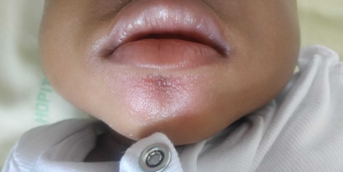
A 14-year-old young man of Chinese origin had been complaining for 1 year of facial erythema that was neither pruritic nor photosensitive, which was a source of concern to those around him but did not particularly bother him. He had always had normal skin, with no notable antecedents or extracutaneous complaints.
Dermatological examination showed a “rough” but not scaly erythema, fairly homogeneous, very well limited over the whole face, reaching the edge of the scalp but respecting the eyelids, the periorificial areas and the median part of the forehead.
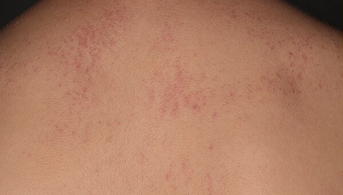
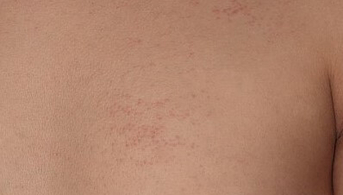
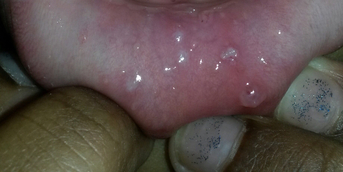
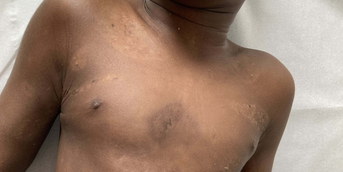
On the extensor surfaces of the arms and thighs, the upper back and décolleté, there were clearly follicular, non-depilating erythematous papules, grouped together in sometimes slightly linear plaques on the upper trunk. Lastly, there was a sometimes slightly papular erythema opposite the metacarpophalangeal and interphalangeal joints on the back of both hands, and a discrete periungual erythema. The rest of the clinical examination, including muscle testing, was strictly normal.
Your turn
What is your diagnosis?
Select 1 answer(s) from the following choices:
Wrong answer!
Good answer!
Selected diagnosis
A connective tissue disease was suggested in the face of this erythema, despite the absence of extracutaneous signs and autoantibodies. Biopsy showed interface dermatitis and a mononuclear infiltrate, as well as a few mucin deposits opposite foci of orthokeratotic hyperkeratosis.
Involvement of the hands (Gottron’s papules) points to dermatomyositis, which can be classified as amyopathic after a negative muscle work-up (enzymes, whole-body MRI). Peripilar enhancement of lesions on limbs and trunk (“keratosis pilaris-like”) is described as Wong’s spiculated dermatomyositis.
This semiological aspect, like the absence of initial muscular involvement, has no prognostic value: muscular involvement may reveal itself clinically at a later stage and should be investigated regularly, as should other systemic involvement (diffuse interstitial lung disease) of the disease.
Explanation of wrong answers
- Ophryogenic erythema is a depilatory red keratosis pilaris affecting the eyebrows. Although it has been described in primary keratosis pilaris, it is particularly suggestive of a RASopathy, and more specifically of cardiofaciocutaneous syndrome, where it is associated with dysmorphia and multiple extracutaneous lesions.
- Atopic keratosis pilaris is a minor sign of atopy associated with mutations in the filaggrin gene. It begins in early childhood and tends to diminish with age. It mainly affects the extensor sides of the arms and thighs and the cheeks. It is always associated with a personal or family history of atopy.
- Pediatric pityriasis rubra pilaris is an acute papular eruption, often very conspicuous, localized preferentially on the posterior surface of the elbows and knees, associated with orange palmoplantar keratoderma and psoriasiform involvement of the face and scalp, which was absent in our case.
Treatment
Treatment with synthetic antimalarials was initially recommended, along with photoprotection.
Message from the expert
Juvenile dermatomyositis is a deceptive disease whose semiologic variants, including Wong’s spiculated form, must be known.
References:
Jason R.Lupton MD, Patricio Figueroa MD, Brenda J. Berberian MD, Virginia I.Sulica MDAn unusual presentation of dermatomyositis: The type Wong variant revisited.
Journal of the American Academy of Dermatology2000; 46: 908-912
Find your clinical cases
Want to read on?
This access is reserved for professionals, registered on Pierre Fabre For Med.
To access the full content, please register or log in if you already have an account.