Elasticity or laxity?
- Connective tissue pathology
-
The clinical case
-
Now it's your turn!
-
Co-prescription and advice
Clinical case presentation
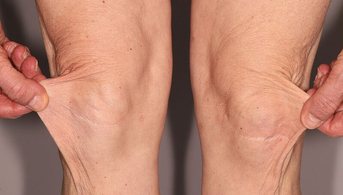
A 50-year-old woman was referred by her plastic surgeon, who was surprised to find abnormal scars on her knees, which had been operated on a few years previously. The patient explained that “her mother had the same skin as her, but was otherwise in very good health”. She herself reported frequent falls as a child, repeated sprains of both ankles and instability of the kneecaps, easy bruising and numerous post-traumatic scars of the face and limbs.
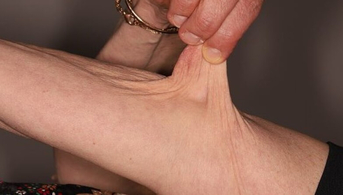
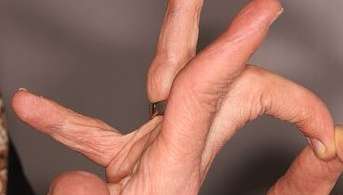
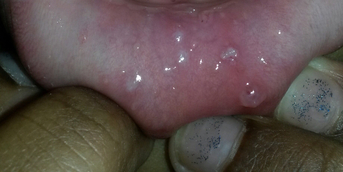
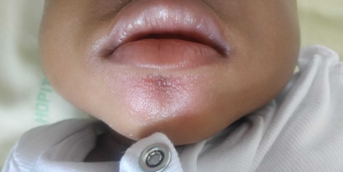
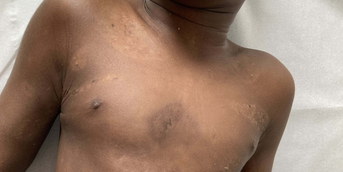
She had practiced ballet for a long time because of her great flexibility but had to stop because of axial and peripheral joint pain. Her obstetric history (three children) was unremarkable. Dermatological examination revealed soft, velvety, hyperelastic skin, especially around the elbows and knees, atrophic papyraceous scars, piezogenic papules and no stretch marks or abnormal skin transparency. There was joint hyperlaxity in all joints: Beighton score (5 joints) = 8/9 and Bulbena score (9 other joint sites) = 9/10.
Your turn
What is your diagnosis?
Select 1 answer(s) from the following choices:
Wrong answer!
Good answer!
Selected diagnosis
This patient presents with skin elasticity with atrophic scarring and generalized joint hyperlaxity, i.e. the two major criteria for the diagnosis of classic Ehlers-Danlos syndrome. A number of minor criteria are also present: soft, flabby skin, easy bruising, skin fragility, repeated dislocations, family history.
The classic type of EDS is the result of autosomal dominant mutations in the COL5A1/2 and COL1A1 genes, characterized by skin hyperelasticity and joint hyperlaxity, with sometimes severe osteoarticular repercussions. Vascular and visceral complications, although far less frequent than in vascular EDS, are not exceptional and should be investigated in a referral center.
Skin biopsy does not provide any evidence in favor of a positive or differential diagnosis. Genetic testing, on the other hand, is indicated and can currently confirm and classify almost all types of EDS, with the exception of the hypermobile form.
Explanation of wrong answers
- Vascular Ehlers-Danlos syndrome is at high risk of serious systemic complications (visceral and vascular ruptures), and its cutaneous signs are dominated by extreme skin fragility (post-traumatic tearing and bruising) rather than the skin and joint hyperelasticity typical of classic Ehlers-Danlos syndrome.
- The cutaneous signs of Marfan syndrome are essentially limited to pathological striae, but it shares joint hyperlaxity with Ehlers-Danlos syndrome.
- Cutis laxa is characterized by cutaneous laxity (flaccid skin), which is the opposite of the hyperelasticity of Ehlers-Danlos syndromes. In the autosomal dominant form, extracutaneous involvement is discreet or absent.
Treatment
The presence of skin fragility in EDS implies:
- preventing situations where there is a risk of hematomas or wounds (contact sports and exposure to trauma) and wearing skin protection,
- tension-free suturing of wounds with non-absorbable thread left in place longer (15 days) and gradually removed (1 stitch in 2).
Message from the expert
It is important not to confuse cutaneous laxity, which translates into “flabby” skin and corresponds to the loss of elasticity seen in cutis laxa, with cutaneous hyperelasticity associated with joint laxity, which points toward Ehlers-Danlos syndromes.
References :
PNDS for non-vascular Elhers Danlos syndrome HAS website
htpps: //www.has-santé.fr 2020
Find your clinical cases
Want to read on?
This access is reserved for professionals, registered on Pierre Fabre For Med.
To access the full content, please register or log in if you already have an account.