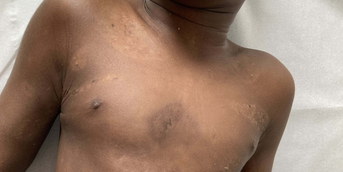
An evocative blue-gray color
- Paediatric dermatology
- Pigmentation disorder
-
The clinical case
-
Now it's your turn!
-
Co-prescription and advice
Clinical case presentation
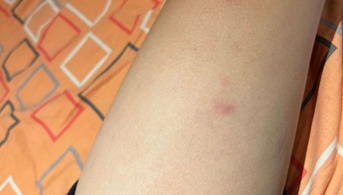
An 11-year-old boy with insulin-dependent diabetes was referred to dermatology for recent lesions on the trunk and roots of the limbs. These lesions, which were neither painful nor pruritic, were erythematous macules evolving over a few days to very superficial secondary desquamation. Questioning revealed no medication other than insulin injections and no history of chemical or thermal injury to the skin.
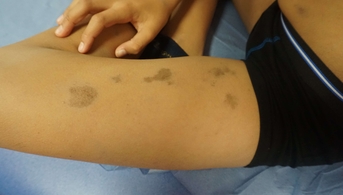
Because of the pauci-lesional and pauci-symptomatic nature of this dermatosis, no assessment or treatment was initially proposed, but rather simple monitoring. Revisited a few weeks later, although the child had not had any recent flare-ups of his dermatosis, large bluish-gray macules were seen, which had succeeded the initial lesions.
Your turn
What is your diagnosis?
Select 1 answer(s) from the following choices:
Wrong answer!
Good answer!
Selected diagnosis
Biopsy of a lesion that was still somewhat inflammatory and already pigmented revealed an interface dermatitis with a perivascular lymphocytic inflammatory infiltrate associated with numerous melanophages. Clinicopathologic correlation is in favor of pigmentary lichen planus.
Pigmentary lichen planus is rarer in children than in adults and, unlike adults, rarely affects the face: lesions are more likely to occur on the trunk and the roots of the limbs and erupt in prepubertal children with a phototype of 4 or above.
Clinical and histologic diagnosis can be difficult when the inflammatory phase has gone unnoticed and examination focuses only on pigmented lesions. The bluish-gray color of the latter is particularly suggestive of this dermatosis, also known as erythema dyschromicum perstans or ashy dermatosis.
Explanation of wrong answers
- Gibert's pityriasis rosea was of course evoked by the initial elementary lesion and the topography of this dermatosis, but a subsequent pigmentogenic evolution has never been reported in this dermatosis.
- Fixed drug eruption is characterized by residual pigmentation of inflammatory lesions, which is “reactivated” each time the incriminating drug is reintroduced. There were no new inflammatory lesions in this child when insulin was continued, which is not a treatment classically associated with this type of drug reaction.
- Idiopathic macular eruptive pigmentation in children is a specific childhood dermatosis that is indistinguishable from a pigmented stage of lichen planus pigmentosus (pigmented macules of the trunk with pigment incontinence on histology), but is never preceded by clinical or histological lesions of lichen.
Treatment
Level IV topical corticosteroid treatment is proposed for active lesions only and not for pigmented sequelae, which should regress spontaneously but very slowly (pigment incontinence).
Message from the expert
As in adults, lichen planus in children can present variable clinical forms, including pigmentary lichen planus, which in this age group tends to affect the trunk rather than the face and is difficult to distinguish from idiopathic eruptive macular pigmentation.
References
Erythema dyschromicum perstans in children: a report of 14 cases. Torrelo A, Zaballos P, Colmenero I, Mediero IG, de Prada I, Zambrano A. J Eur Acad Dermatol Venereol. 2005 Jul;19(4):422-6.
https://pubmed.ncbi.nlm.nih.gov/15987286/
Systematic Review of Lichen Planus Pigmentosus in Children.
Mitchell K, Silverberg N.J Drugs Dermatol. 2022 Aug 1;21(8):850-853
Find your clinical cases
Want to read on?
This access is reserved for professionals, registered on Pierre Fabre For Med.
To access the full content, please register or log in if you already have an account.