False ichthyosis
- Paediatric dermatology
-
The clinical case
-
Now it's your turn!
-
Co-prescription and advice
Clinical case presentation
A 7-year-old girl with atopic disease (eczema and asthma) had been complaining for 1 year of severe muscle fatigue on exertion and pain in both lower limbs.
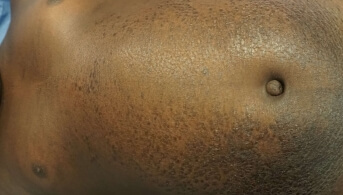
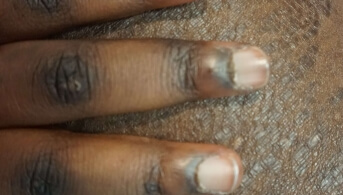
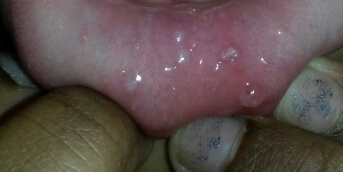
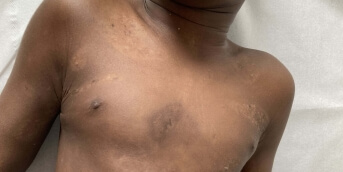
The laboratory work-up was normal apart from a sharp rise in CPK. Later, a skin presentation completely different from her long-standing and well-known atopic dermatitis developed: ichthyosiform plaques discreetly infiltrated from the abdomen to the roots of all four limbs, associated with pigmentation of the eyelids and an infiltrated and keratotic appearance of the nail folds on the fingers (photos 1, 2, 3).
Muscle testing remained abnormal, as did CPK levels. MRI and muscle biopsy showed diffuse muscle inflammation. Skin biopsy revealed a dermal inflammatory infiltrate and nonspecific calcium deposits.
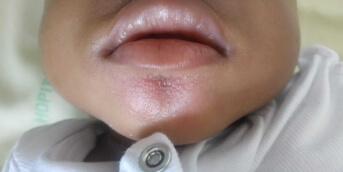
Finally, Mi-2 antibodies were positive. Intensive immunosuppressive therapy (systemic corticosteroids and JAK inhibitors) led to resolution of muscle symptoms and improvement of skin signs but did not prevent the appearance of calcinosis plaques in previously ichthyosiform areas (photo 4).
Your turn
What is your diagnosis?
Select 1 answer(s) from the following choices:
Wrong answer!
Good answer!
Selected diagnosis
This juvenile dermatomyositis (JDM) complicated by cutaneous carcinomatosis is interesting for its atypical dermatological presentation.
While pigmentation of the eyelids (possibly equivalent to erythema on phototype V) and periungual involvement (“manicure sign”) were suggestive in this context of muscular involvement, an ichthyosiform appearance is very rarely described in dermatomyositis (DM).
Most of the few published cases concern paraneoplastic DM in adults, bearing in mind that progressive cancer is also a classic cause of acquired ichthyosis.
Childhood DM is never paraneoplastic and calcium deposits were already present on biopsy of the initial skin lesions.
Explanation of wrong answers
Dorfman-Chanarin syndrome is a syndromic genetic ichthyosis, as it is part of a metabolic disease that also affects the liver and muscles (myopathy). Ichthyosis is congenital, in the form of severe non-bullous ichthyosiform erythroderma that persists throughout life.
Ichthyosis vulgaris should, of course, be considered in the context of atopy, but it begins around the age of 6 months, predominates on the lower limbs in the form of fine white scales, and is not syndromic apart from various allergic manifestations.
A paraneoplastic cause should be systematically considered in any acquired ichthyosis, as should an infectious cause, but the extracutaneous context in this child obviously suggests another type of pathology.
Treatment
This is the usual immunosuppressive treatment for dermatomyositis, discussed in the RCP of pediatric internal medicine, and in this case it is an intensive treatment due to the severity of the muscle damage.
However, there is currently no consensus on the curative treatment of cutaneous calcinosis.
Message from the expert
Cutaneous calcinosis secondary to JDM can occur very early in the course of the disease and is not always responsive to the various treatments.
References:
Wendel S, Venhoff N, Frye BC, May AM, Agarwal P, Rizzi M, Voll RE, Thiel J. J Successful treatment of extensive calcifications and acute pulmonary involvement in dermatomyositis with the Janus-Kinase inhibitor tofacitinib - A report of two cases.
Autoimmun. 2019 Jun;100:131-136.
Find your clinical cases
Want to read on?
This access is reserved for professionals, registered on Pierre Fabre For Med.
To access the full content, please register or log in if you already have an account.