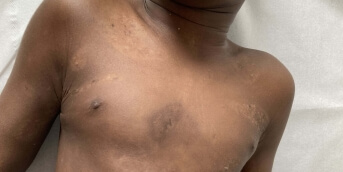
A febrile pustular rash
- Dermatological impact of a general disease
-
The clinical case
-
Now it's your turn!
-
Co-prescription and advice
Clinical case presentation
This 13-year-old boy has a history of psoriasis in a grandfather but not in his parents, who are not related. He was treated for asthma between the ages of 3 and 6 but has never had eczema.
His dermatosis began abruptly with a scaly scalp, in a non-infectious context. A bilateral inguinal intertrigo and inflammatory, pruritic polycyclic plaques on the trunk and four limbs soon appeared.
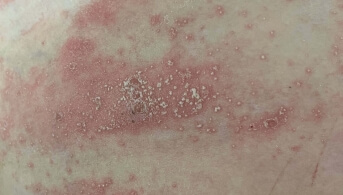
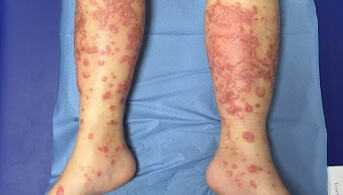
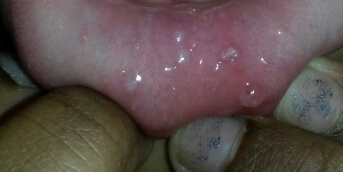
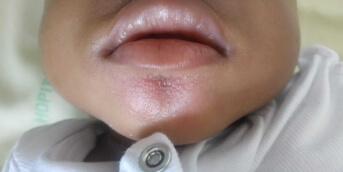
His dermatosis rapidly escaped intensive topical corticosteroid therapy, and he was hospitalized because it had become pustular, almost erythrodermic (including palms and soles), accompanied by fever, edema of both lower limbs and cutaneous, muscular and joint pain.
There is no viral background and no history of medication use. Biopsy confirmed neutrophilic pustulosis of the stratum corneum, associated with parakeratosis and a polymorphic inflammatory infiltrate of the superficial dermis. Biological tests showed neutrophilic hyperleukocytosis and an inflammatory syndrome. Cutaneous microbiological samples were negative.
Your turn
What is your diagnosis?
Select 1 answer(s) from the following choices:
Wrong answer!
Good answer!
Selected diagnosis
Biopsy confirmed the diagnosis of generalized pustular psoriasis (GPP), the first diagnostic hypothesis for this aseptic neutrophilic pustulosis in the absence of drug intake.
GPP is a very rare form of psoriasis in children and, as in adults, often includes a systemic dimension (fever, arthralgia, myalgia, inflammatory syndrome, systemic neutrophilic involvement) which worsens the prognosis. A genetic sample taken from the child and his parents to rule out monogenic GPP was negative.
Explanation of wrong answers
- Negative mycological samples (scalp, trunk lesions) rule out generalized dermatophytosis favored by topical corticosteroid therapy.
- Acute generalized exanthematous pustulosis is a severe toxidermia that sometimes poses a problem of differential diagnosis with GPP but can be easily ruled out in the absence of any treatment prior to the eruption.
- Generalized pustular dermatophytid reaction occurs when systemic antifungal therapy is initiated in the context of ringworm and corresponds to a type IV immunological reaction to fungal antigens.
Treatment
Treatment with acitretin was started with initial improvement. After 1 month of treatment, remission was very partial and a switch to adalimumab was proposed.
There is no consensus on the treatment of GPP in children, but a recent review of the literature suggests rapid recourse to biologic therapies, possibly combined with conventional non-biological treatments such as acitretin, ciclosporin or methotrexate.
Message from the expert
The identification of pathogenic variants in the GPP genes (IL36RN, CARD14 and AP1S3) is all the more frequent when GPP is associated with acrodermatitis continua of Hallopeau and not with plaque psoriasis.
References:
Muskaan Sachdeva and col Management of pediatric generalized pustular psoriasis using biologics: An evidence-based review JAAD 2022; 87: 484-486
Find your clinical cases
Want to read on?
This access is reserved for professionals, registered on Pierre Fabre For Med.
To access the full content, please register or log in if you already have an account.