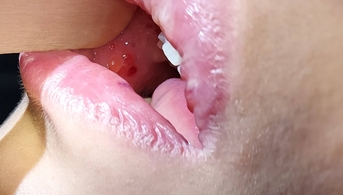
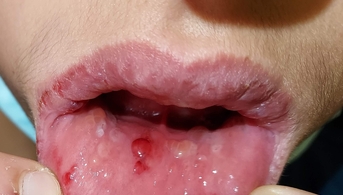
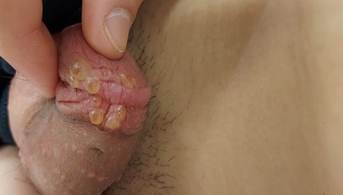
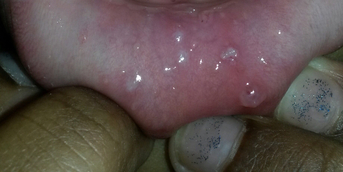
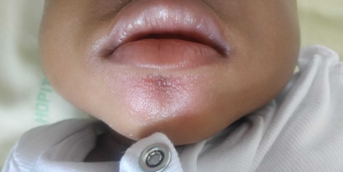
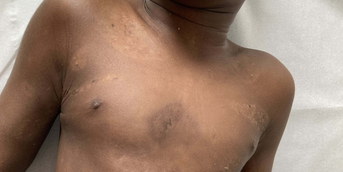
Initial mucosal bullae
- Mucosal pathology
-
The clinical case
-
Now it's your turn!
-
Co-prescription and advice
Clinical case presentation
This adolescent presented to the emergency department with tense, painful bullous lesions of the oral mucosa, lips and preputial sulcus; he also complained of odynophagia, urinary burning and ocular pruritus. He had not taken any oral or topical medication in the days preceding the eruption, was not febrile and had no infectious complaints.
His history included hospitalization at the age of 7 for a mucocutaneous rash concurrent with a Mycoplasma pneumoniae infection (positive IgM and IgG serology) and several episodes of painful erosive stomatitis labeled “herpetic stomatitis.”
Hospitalized for assessment, urinary catheterization and infusion of analgesics, he rapidly developed vesiculobullous lesions with an erythematous halo on the skin.
Oral and ENT examination revealed crusted, hemorrhagic cheilitis, multiple erosions of the oral cavity and bullous detachment of the soft palate and posterior pharyngeal wall. Ophthalmologic examination showed simple conjunctivitis without keratitis. Herpes serology was negative, as was Mycoplasma PCR. Complete healing of all lesions, without sequelae, occurred only after 3 weeks of purely symptomatic treatment.
Your turn
What is your diagnosis?
Select 1 answer(s) from the following choices:
Wrong answer!
Good answer!
Selected diagnosis
Despite the absence of any real “target lesions,” we clinically retained the diagnosis of idiopathic recurrent mucocutaneous erythema multiforme in light of this recurrent mucocutaneous bullous eruption with long intervals of spontaneous remission.
Negative herpes serology formally rules out post-herpetic recurrent erythema multiforme, and there was no evidence of a new Mycoplasma infection during the last episode.
Explanation of wrong answers
- Bipolar herpes: Primary infection with bipolar HSV-1 (oral and genital mucosa) or disseminated cutaneous HSV-1 (eczema herpeticum) is possible, but disseminated mucocutaneous HSV-1 is not likely to occur outside a context of severe immunodepression. Furthermore, mucosal lesions are bullous rather than vesicular and HSV-1 serology is negative (although this may be seen in the early stages of primary infection).
- Linear IgA bullous dermatosis, or LABD: This is the most common autoimmune bullous dermatosis (AIBD) in children, manifesting as skin involvement classically described as taut, rosetted bullae of ubiquitous but frequently bipolar topography (face and external genitalia). Mucosal involvement is possible in LABD, but when it is in the foreground and also affects ophthalmologic and ENT mucosa, another AIBD of the bullous pemphigoid group should be considered. In our case, the recurrent nature of the bullous dermatosis, interspersed with long periods of spontaneous remission, does not suggest AIBD.
Treatment
In the absence of a consensus on the indication for treatment of erythema multiforme outbreaks with corticosteroids, treatment remained symptomatic with hygiene care, intravenous analgesics, nutritional support (liquid protein and energy supplements) and prevention of ophthalmologic and genital mucosal complications.
Given the negativity of the herpes serology, no preventive treatment against recurrence was proposed.
Message from the expert
Erythema multiforme may begin as a uni- or multifocal mucosal, vesiculobullous or erosive condition, the diagnosis of which is not always obvious in the absence of characteristic cutaneous lesions.
References
Triggers, clinical manifestations, and management of pediatric erythema multiforme: A systematic review.
Zoghaib S, Kechichian E, Souaid K, Soutou B, Helou J, Tomb R.J Am Acad Dermatol. 2019 Sep;81(3):813-822
Find your clinical cases
Want to read on?
This access is reserved for professionals, registered on Pierre Fabre For Med.
To access the full content, please register or log in if you already have an account.