Sore gums
- Mucosal pathology
- Paediatric dermatology
-
The clinical case
-
Now it's your turn!
-
Co-prescription and advice
Clinical case presentation
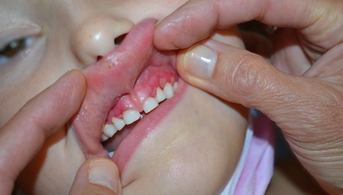
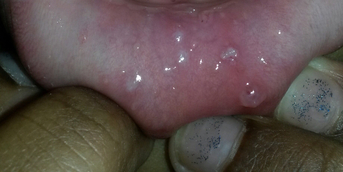
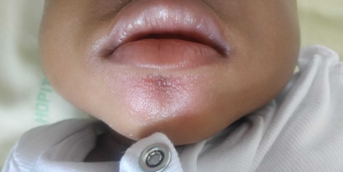
This 7-year-old girl had been suffering from painful, hemorrhagic gingivitis for several months. She had no personal or family history, including in terms of autoimmune diseases, and was taking no medication. Despite eating difficulties related to her oral lesions, she maintained a balanced diet and a satisfactory growth curve.
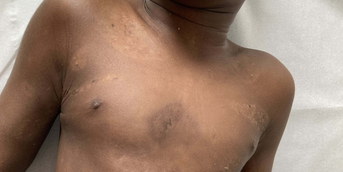
Intraoral examination showed exclusive gingival involvement (attached gingiva), while the labial and buccal mucosa were unaffected. The gingiva was inflamed and erosive in places, with a "Nikolsky sign." All other mucous membranes were unaffected, including after extensive ophthalmologic and ENT examinations. The patient had already had several normal blood workups and undergone several scaling procedures under the hypothesis of tartar-related gingivitis. A gingival biopsy was performed under local anesthesia in stomatology.
Your turn
What is your diagnosis?
Select 1 answer(s) from the following choices:
Wrong answer!
Good answer!
Selected diagnosis
Histological examination of the gingival mucosa revealed an incipient subepidermal split and a dermal inflammatory infiltrate rich in plasma cells and eosinophils. Direct immunofluorescence was positive, with linear deposition of IgG and C3 at the dermoepidermal junction.
Indirect immunofluorescence, ELISA and immunoblot were negative. This is therefore a junctional autoimmune bullous dermatosis with exclusive gingival involvement in a child with no known immune disorder. The workup favored mucous membrane pemphigoid, although acquired epidermolysis bullosa cannot be formally ruled out. The absence of G6PD deficiency and poor prognostic factors (no ophthalmologic or ENT involvement) led to first-line treatment with dapsone, introduced at a progressively increasing dose. At dose of just 1 mg/kg/day, a clear improvement in lesions was observed.
Explanation of wrong answers
- Primary HSV-1 infection, when symptomatic in children, manifests as an acute, highly painful, vesicular and then erosive gingivostomatitis, most often associated with perioral vesicles and high fever. It heals spontaneously in about ten days, and recurrences usually take the form of a labial cold sore. Intraoral recurrences are rare, localized and occur in flare-ups.
- Mucosal, and therefore oral, involvement of lichen planus is exceptional in children, even more so for its erosive form. In adults, erosive gingival lichen planus is clinically indistinguishable from mucous membrane pemphigoid or acquired epidermolysis bullosa and is therefore a histological diagnosis.
- Recurrent erythema multiforme of the oral mucosa occurs in children, but the erosive lesions, which are often very pronounced, involve the entire oral mucosa and occur in flare-ups interspersed with complete remission, which was not the case in this patient.
Treatment
Given the functional risks involved (blindness, laryngeal and esophageal stenosis), the therapeutic management of mucous membrane pemphigoid falls within the remit of a multidisciplinary team specializing in autoimmune bullous dermatoses. The first-line treatment in children remains dapsone and topical corticosteroid therapy, but intensification of immunosuppressive therapy should be discussed in the event of treatment failure or inadequate control.
Message from the expert
In both children and adults, erosive gingivitis should raise suspicion of autoimmune bullous dermatosis, even in the absence of associated skin lesions.
References
Rodriguez Baisi K, Wentworth A, Chattha AJ, DiCaudo DJ, Mangold A, Nelson SA, Siegfried E, Wieland CN, Tollefson MArare case of childhood mucous membrane pemphigoid involving the oral and genital mucosa. Pediatr Dermatol. 2021;38(4):904-907
Find your clinical cases
Want to read on?
This access is reserved for professionals, registered on Pierre Fabre For Med.
To access the full content, please register or log in if you already have an account.