Rough skin and photophobia: the right mix
- Paediatric dermatology
-
The clinical case
-
Now it's your turn!
-
Co-prescription and advice
Clinical case presentation
A 7-year-old boy has an oral processing disorder and numerous food phobias in the context of severe autism. He has phototype IV and no personal or family history of atopy. He was born with normal skin.
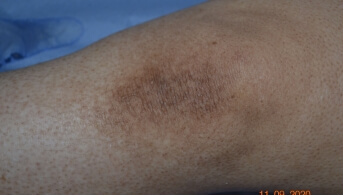
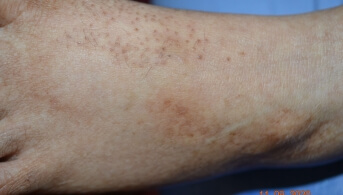
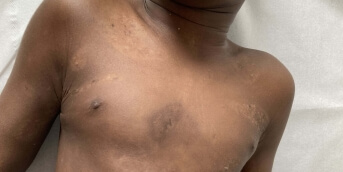
Over the past few months, the parents had noticed that the skin on his four limbs and buttocks had become rough, with a tendency toward hyperpigmentation of the same distribution.
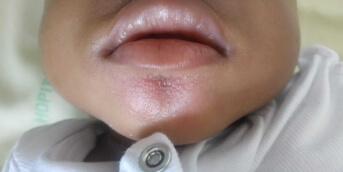
The child had also recently been undergoing ophthalmological treatment for photophobia, which had led to the discovery of keratoconjunctivitis that responded poorly to lubricating eye drops.
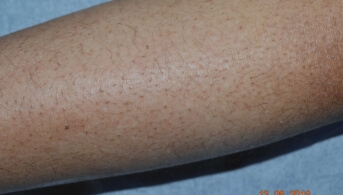
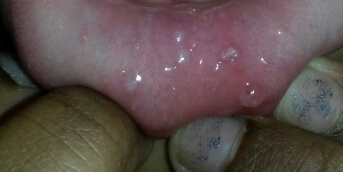
Dermatological examination revealed keratosis pilaris, predominantly on the extensor surfaces of the lower limbs, associated with a dirty brown discoloration over bony prominences. There were no abnormalities of the skin appendages or oral mucosa, and no tendency to bruising.
Your turn
What is your diagnosis?
Select 1 answer(s) from the following choices:
Wrong answer!
Good answer!
Selected diagnosis
The sporadic, profuse, late-onset nature of this keratosis pilaris, in the absence of an associated history or malformative syndrome, suggests an non-genetic underlying cause. The psychiatric background and secondary malnutrition immediately suggest a nutritional deficiency disorder.
The vitamin workup confirmed a severe vitamin A deficiency, suggested clinically by this phrynoderma appearance, associated with hyperpigmentation and ocular epithelium involvement.
Vitamin A deficiency is relatively rare. It may be secondary to malabsorption (pancreatic insufficiency) or an unbalanced diet (insufficient vegetables and dairy products), as in this child with an oral processing disorder.
Explanation of wrong answers
- This is not atopic keratosis pilaris (filaggrin gene mutation): no family or personal history of atopy, no other minor cutaneous signs of atopy, and the condition is acquired.
- The absence of a polymalformative syndrome (heart disease, facial dysmorphia, short stature) does not support a RASopathy, particularly cardio-facio-cutaneous syndrome, in which keratosis pilaris also affects the face and is frequently erythematous and depilating (ulerythema ophryogenes).
- The non-purpuric nature of this keratosis pilaris and the absence of hair abnormalities and gingivitis argue against scurvy, consistent with a normal plasma vitamin C level.
Treatment
Intravenous followed by oral vitamin A supplementation corrected the cutaneous and ophthalmological signs. It should be continued long term in this context.
Message from the expert
Acquired xerosis may classically suggest a nutritional problem, but keratosis pilaris points more specifically to vitamin A deficiency.
References :
Deficiency dermatoses. In: Bessis D, Francès C, Guillot B, Guilhou JJ (Éds), Dermatologie et Médecine, vol. 4: Manifestations dermatologiques des maladies d'organes. Springer-Verlag France, 2011:77.1-77.8
Find your clinical cases
Want to read on?
This access is reserved for professionals, registered on Pierre Fabre For Med.
To access the full content, please register or log in if you already have an account.